What are the treatment options for brain cancer?
The treatment options for brain cancer may include surgery, chemotherapy, radiotherapy, targeted therapies and steroid therapy, alongside new and evolving treatments through clinical trials. The type of treatment you receive will depend on several different considerations, such as the type of brain cancer you have, its stage, your overall health and your treatment preferences. This page aims to give you a comprehensive overview of how brain cancer treatment works.
Surgery for brain cancer
Surgery is a common treatment option for many people with brain cancer. Surgery is performed for brain cancer patients to remove cancerous tissue and relieve or prevent symptoms from the brain tumour, such as any impact on normal functions (e.g. speech, vision, movement). For people who do not receive surgery or who require further treatment following surgery, other treatments such as radiotherapy, chemotherapy or targeted therapies may be required.
Craniotomy
A craniotomy is the most common type of surgery for brain cancer, which involves the partial or complete removal of the brain tumour by removing a piece of skull in the brain. The section of skull is then replaced with small plates and screws following the surgery.
The three approaches for craniotomy include:
-
Craniotomy using general anaesthetic
This procedure is performed under general anaesthetic. General anaesthesia is used during high-precision tumour removal to ensure you do not move when there is no risk of damage to areas of your brain that control speech, vision or movement.
-
Computer guided (stereotactic) craniotomy
This procedure uses a computer navigation system to guide the surgery, allowing greater precision. In comparison to non-computer guided craniotomy, this procedure is less invasive and offers greater accuracy and safety for patients.
-
Awake craniotomy
This procedure is performed using local anaesthetic, which means that you will remain awake during the surgery and can speak, move and respond, but won’t feel pain. An awake craniotomy may be recommended if the cancer is near a location that controls vision, speech or movement to avoid damaging these areas and monitor your brain activity throughout the surgery
Endoscopic transsphenoidal surgery
Endoscopic transsphenoidal surgery is a minimally-invasive procedure, which involves removing brain tumours located at the base of the brain using an endoscope. This involves the insertion of the endoscope through the nose and into the skull at the base of the brain to access and remove the tumour. It is the most common type of surgery people with brain cancer near the base of the brain (such as pituitary gland tumours).
Laminectomy
A laminectomy is a common treatment for tumours in the spinal cord and involves the removal of your tumour through an incision in the skin, muscle and vertebra in the spine. This procedure also helps to relieve pressure on the spinal cord and symptoms caused by the tumour (such as pain or weakness).
Radiotherapy for brain cancer
Radiotherapy is a common treatment for brain cancer and is often given after surgery, as an alternative to surgery or alongside other treatments. There are many different radiotherapy techniques that may be suitable for your brain cancer.
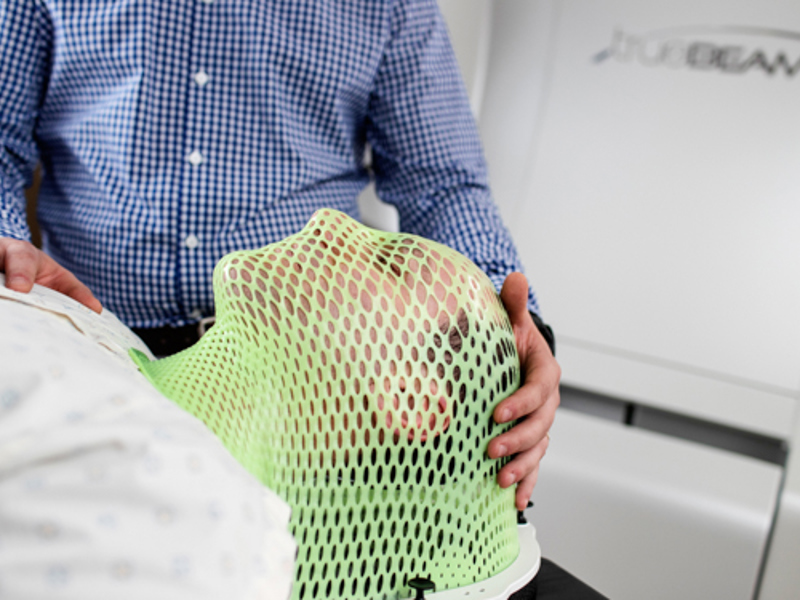
Immobilisation devices
If you receive radiotherapy for your brain cancer, you may also need an immobilisation device such as a mask to ensure you stay as still as possible throughout your treatment.
Learn more about immobilisation masks and how they are made.
External beam radiotherapy
External beam radiotherapy (EBRT) is used to treat brain cancer by delivering highly targeted radiotherapy beams directly to the tumour/s in your brain.
Types of EBRT which can be used for the treatment of brain cancer include:
Image guided radiotherapy (IGRT) is used to ensure EBRT is delivered as accurately as possible to your brain cancer. This involves the use of advanced imaging equipment and computer software such as MRI, CT and x-ray.
Stereotactic radiosurgery
Stereotactic radiosurgery (SRS) is a specific type of targeted radiotherapy that can be used to treat small benign or malignant (cancerous) brain tumours and tumours that can’t be treated with surgery or that have metastasised (spread to the brain from other areas of the body). Benign tumours which may be treated using SRS include meningiomas, pituitary adenomas and acoustic neuromas as well as some blood vessel conditions such as arteriovenous malformations.
SRS involves a special type of high-dose radiotherapy that targets affected areas in the brain while avoiding healthy brain tissue, and is usually delivered in one to five treatments.
At Icon, we use state-of-the-art technologies which can deliver SRS treatment to multiple brain tumours at the same time. This reduces the need to treat multiple tumours separately, resulting in a much shorter treatment time for patients.
Listed below are two examples of software used to help deliver this advanced treatment. Other technologies may be used to treat multiple tumours, depending on the location of your treatment centre, but the software all work to achieve the best possible outcomes for patients.
Varian HyperArc – HyperArc technology is available at Icon Canberra, Icon Greenslopes, Icon Gold Coast Private and Icon Maroochydore
BrainLab Elements – BrainLab Elements is used at Icon Richmond and Icon Mulgrave
Stereotactic radiotherapy
Stereotactic radiotherapy (SRT) is an advanced technique used to treat malignant (cancerous) and benign tumours with well-defined edges in the brain. SRT is similar to SRS, but is usually delivered over a longer course of treatment and is more commonly used for larger lesions (tumours), especially those that are in sensitive areas of the brain.
Compared to traditional radiotherapy to the brain, which involves treating the entire brain, stereotactic radiotherapy only targets the individual tumours with high doses of radiation. This provides less radiation to healthy brain tissue, reducing the impact of side effects (e.g. loss of intellectual function, hair loss and headaches) and improving the quality of life for patients.
Chemotherapy for brain cancer
Chemotherapy uses a range of drugs to kill and slow the growth of brain cancer cells and is primarily used for faster-growing brain cancers. It may be given following surgery or in combination with radiotherapy (known as chemoradiation).
Learn more about chemotherapy and how it is delivered.
Chemotherapy treatment for brain cancer takes place over several sessions, which is known as a cycle. Your care team will walk you through how many cycles you may need for your course of treatment, with most people completing chemotherapy in a period of three to six months.
Common chemotherapy medicines
Using chemotherapy drugs to treat brain cancer can be difficult due to the blood brain barrier, which is an ‘in built’ protection system stopping harmful substances in the blood from reaching the brain. Only some types of chemotherapy drugs can effectively get through the blood brain barrier.
Chemotherapy drugs that may be used to treat brain cancer include:
-
This drug works by damaging the DNA within cells so that they are unable to divide and grow. This affects cancer cells since they grow more rapidly than normal healthy cells. Temozolomide is usually given as a course together with radiotherapy and is taken orally as a tablet once daily.
-
This is a combination of three chemotherapy drugs that are commonly used together to treat brain cancer before radiotherapy. Vincristine is given by intravenous infusion, while procarbazine and lomustine are both given orally as a tablet.
Targeted therapies for brain cancer
Targeted therapy is a less common treatment option for brain cancer which uses specialised drugs to destroy specific proteins in brain cancer cells.
Targeted therapy drugs that may be used to treat brain cancer include:
Bevacizumab - This is a monoclonal antibody that targets and blocks a specific protein on cancer cells called VEGF (vascular endothelial growth factor), which promotes the growth of blood vessels that supply essential nutrients to cancer cells. When VEGF is blocked, cancer cells no longer receive the essential nutrients and oxygen that they need to grow and survive. It is used to treat advanced and recurrent brain cancer and is given by intravenous infusion every 14 days, with each infusion taking around 30-90 minutes.
Steroid therapy for brain cancer
Steroid therapy may be used for people with brain cancer who are experiencing swelling in the brain due to the size and location of their brain tumour or as a side effect from their treatment. It can be given at any point during treatment, including before, during or after surgery and radiotherapy, to reduce this swelling and relieve any associated symptoms (such as headaches).
Steroid therapy drugs which may be used to treat brain cancer include:
Dexamethasone - This is a tablet that is taken to help reduce inflammation and swelling in the brain caused by brain cancer. When people take steroids over a period of time (several months), they can experience side effects such as puffiness in the face, feet or hands, increased blood sugar, high blood pressure, osteoporosis, poor wound healing and increased risk of infection. Your care team will monitor your progress and may modify your treatment to help manage any side effects you may experience.
Clinical trials for brain cancer
Icon offers a wide range of clinical trials providing patients with access to new and evolving treatments. Clinical trials offer hope and opportunity and contribute to breakthroughs in treatment for future cancer patients.

Treatment by grade of brain cancer
When you are diagnosed with brain cancer, your oncologist will develop your treatment plan as part of a multidisciplinary team based on the grade of your cancer.
Common treatment options for each grade of brain cancer include:
Grade I brain cancer
Surgery is usually the only treatment needed for grade I brain cancers, however stereotactic radiosurgery (SRS) and stereotactic radiotherapy (SRT) may be used as an alternative to surgery for some brain cancer patients. Chemotherapy is sometimes used as a treatment option when is surgery is not possible.
Grade II brain cancer
Grade II brain cancer is commonly treated using surgery, however it may also require further treatment. This typically includes radiotherapy treatment followed by chemotherapy treatment.
Grade III brain cancer
Treatment for grade III brain cancer typically involves surgery followed by chemotherapy and radiotherapy.
Grade IV brain cancer
Grade IV brain cancer is typically treated using surgery alongside chemotherapy and radiotherapy. A targeted therapy may also be used for advanced brain cancer, but only after radiotherapy and chemotherapy have first been tried.










