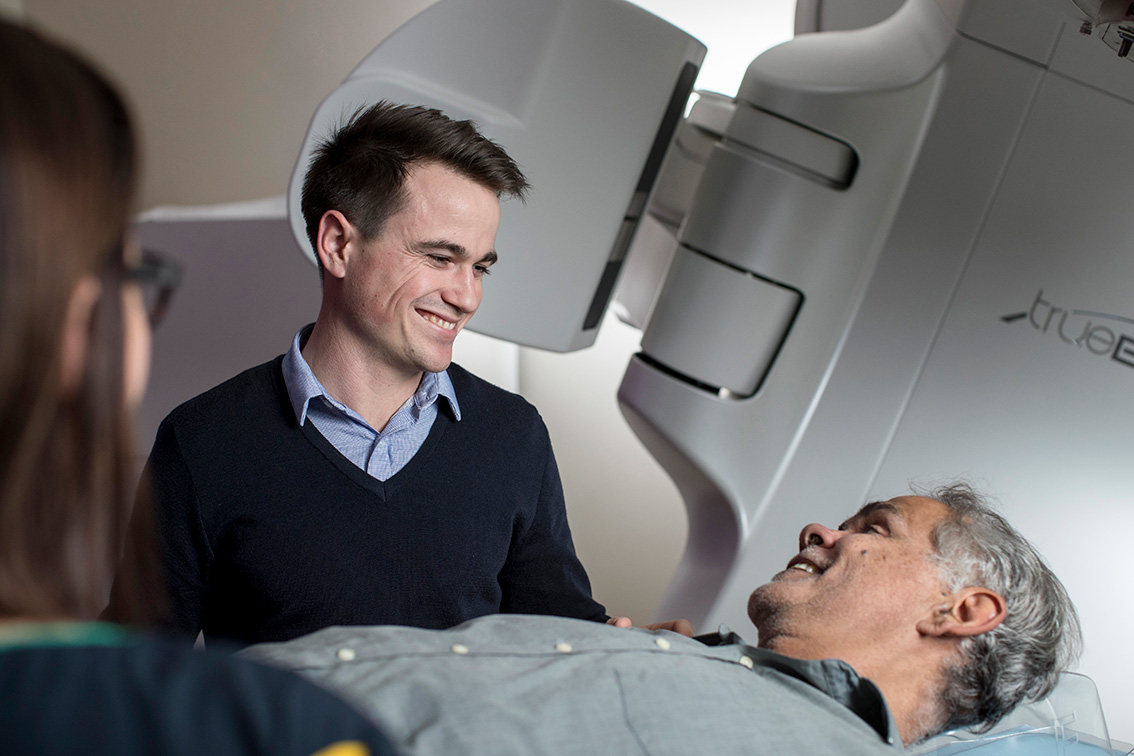
The immune system is made up of cells and organs that protect the body from threats such as infections, toxins and abnormal cell growth. The immune system recognises when a foreign organism, such as a germ, enters the body and attacks it to stop it from harming the body.
Immunotherapy, or biologic therapy, is a type of treatment that uses your own immune system to fight cancer.
While not as commonly used as surgery, chemotherapy, or radiation therapy, immunotherapy in Australia is rapidly becoming a key treatment option for a wide range of cancers. It offers life-extending or lifesaving outcomes for many patients.